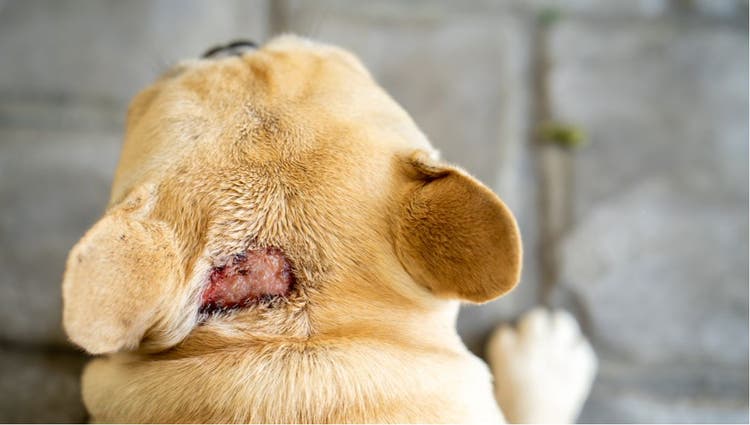
Acute Moist Dermatitis (Hot Spots) in Dogs
Overview of Canine Hot Spots
Acute moist dermatitis, also commonly known as “hot spots” or “pyotraumatic dermatitis,” are acute, moist, localized, inflamed, and rapidly progressive bacterial infections of the skin. Acute moist dermatitis is a very common skin disease for dogs.
The precise sequence of events leading to hot spots is not known, but anything that can initiate an itch-scratch cycle can lead to this condition. The sequence most likely begins with something that irritates the skin and the body’s response is either to itch or become inflamed. The inflammation then causes the dog to lick or chew the area, which further damages the skin, and creates a cycle of self-trauma from itching, scratching, and chewing.
Common Causes
The most common skin irritant that causes hot spots is fleas.
Other reasons for hot spots include:
- Allergies (flea allergy, atopy, contact, or food allergy)
- Parasitic diseases (sarcoptic and demodectic mange)
- Anal gland disease
- Poor grooming or an unkempt coat
- Insect bites (ticks, bees, and mosquitos)
- Burrs
- Minor wounds
- Outer ear infections (otitis externa)
- Summer heat
- Excessive moisture such as from swimming
- Irritation that develops after clipping and grooming
Less common causes of hot spots include ringworm (dermatophytosis), drug reactions, autoimmune disease (where the body fails to identify self-components and reacts against normal tissues), and vasculitis (inflammation of blood vessels).
Hot spots are most common in dense, long-haired, and heavy-coated breeds, and are more prevalent during the summer months. Typical locations for “hot spots” are the sides of the face, around the neck, dorsal back, and the flank (lateral thigh). They can occur in any breed, but are more common in Golden Retrievers, Labrador Retrievers, St. Bernards, and German Shepherds. Young dogs (less than 4 years old) seem to be predisposed. It is rarely diagnosed in cats.
The role of bacteria in the development of hot spots is also unclear. Some cases of acute hot spots seem to be initiated by folliculitis (inflammation and infection of hair follicles), and this seems to be common in St. Bernards and Golden Retrievers. Other affected dogs do not seem to have an important bacterial component and respond to clipping of the hair, cleansing of the skin, and corticosteroid therapy.
Key Points about Hot Spots
- The lesions of acute moist dermatitis are reddened (erythematous), swollen, and hairless. They exude a discharge and are extremely painful. Their onset and progression are rapid. Pruritus (itchiness) is intense, and severe self-trauma can cause lesions in a very short period of time.
- Two types of acute moist dermatitis occur. One type does not have an important bacterial component and manifests as a superficial ulcerated plaque. The second type, in addition to being an ulcerated plaque, also has peripheral papules (small reddened bumps) suggestive of bacterial folliculitis.
- Typical locations of hot spots are the hindquarters and the sides of the face below the ear. Lesions on the hindquarters usually are caused by underlying flea allergy, whereas those on the side of the face are usually associated with concurrent ear inflammation (otitis) secondary to allergies.
What to Watch For
Clinically, the lesions of acute hot spots are secondary to self-inflicted trauma. Strangely, even severe self-trauma in some dogs will not create a hotspot, while in others, minimal self-trauma may do so.
Typically, dogs with hot spots will exhibit the following:
- Areas of hair loss with clearly demarcated, red, inflamed skin that is moist and oozing.
- Matted hair around the lesion.
- Crusty or scabbed skin.
- Intense scratching.
- Lesions, which can expand quickly (often within minutes to hours). Single lesions are more common than multiple areas of involvement.
- Areas of extreme pain (with some benign animals becoming aggressive with lesion manipulation).
Diagnosis of Hot Spots in Dogs
Diagnosis of hot spots is generally based on history, clinical signs, and physical examination. Diagnostic tests may be needed to confirm the diagnosis and exclude other diseases. However, your veterinarian can usually make a preliminary diagnosis based on a history of rapid onset and the clinical appearance of the lesions.
Tests to evaluate for other or related diseases may include:
- Skin scrape testing, which is important to rule out demodectic or sarcoptic mange as a possible underlying cause.
- Microscopic examination of smears from the exudate is useful to identify a bacterial component. If bacterial infection (pyoderma) is present, degenerate neutrophils (a type of white blood cell) with bacteria (usually Staphylococci) inside of them are often found.
- A diagnostic evaluation for flea allergy and other allergies (an elimination food trial) should be performed if the animal has a long history of acute hot spots. Examination of ear exudate in dogs with facial lesions and concurrent ear infections is important to identify the organism (bacteria or yeast) and properly treat the underlying cause of infection.
- Skin biopsy is often recommended in lesions that are not responsive to traditional therapies.
Hot Spot Treatment Options
Treatment for hot spots may include one or more of the following:
- Clipping and cleaning of the affected area. Lesions are often more extensive than they initially appear. Clipping the hair in the area is important to allow proper cleaning of the affected skin to remove crusts and exudate. Antibacterial solutions (chlorhexidine) or drying solutions (Burrow’s solution) combat infection and decrease pruritus (itchiness). Because these lesions can be extremely painful, sedation is sometimes required to properly treat the affected area.
- Topical Astringents. Small lesions may be treated topically with astringents such as 2% aluminum acetate solution or a combination of steroid and antibiotic creams or gels. Antipruritic sprays containing hydrocortisone, lidocaine, or pramoxine are also helpful, but short-acting.
- Interruption of the pruritic (itch) cycle. This is crucial to successful treatment. Once the cycle has been triggered, it is important to stop it so as to prevent self-mutilation.
- Orally-administered cortisone-like drugs (glucocorticoids such as prednisone) are often used for a short period of time, such as 5 to 10 days, to make the dog more comfortable. Dogs may be more hungry and thirsty while receiving corticosteroids, which is a common side effect of this medication. As a consequence, the dog may need to urinate more frequently than normal. Some dogs may even pant in relation to corticosteroid therapy.
- An alternative to steroids is nonsteroidal anti-inflammatory drugs (carprofen or meloxicam) for pain management. These drugs cannot be given at the same time as glucocorticoids.
- Oclacitinib, commonly known by the brand name Apoquel®, is an oral medication that has proven effective at controlling itching without the side effects of steroids.
- Cytopoint®, also known by the names Lokivetmab and Canine Atopic Dermatitis Immunotherapeutic (commonly abbreviated as CADI), is a monoclonal antibody treatment that targets and deactivates the itch signal to the brain.
- Oral Antibiotics. In some cases, damage is so extensive that bacteria proliferate, resulting in secondary infection, which must be treated if present. In such instances, oral antibiotics may be prescribed for 2 to 3 weeks. A commonly used antibiotic is Cephalexin (Keflex®). Antibiotic therapy for a minimum of three weeks may be necessary in animals with secondary bacterial folliculitis.
- Elizabethan collars (E-collars) can put a stop to self-trauma. These collars are made of large sheets of plastic material that encircle the pet’s neck and prevent them from licking or biting their skin. They should be worn at all times until otherwise directed by your veterinarian. T-shirts may be used to loosely cover a hot spot and may be an alternative to an e-collar, depending on the location of the wound and the personality of the dog.
- Flea control. If possible, identification and treatment of the underlying cause is important to prevent recurrent episodes. Most cases are secondary to flea allergy and aggressive flea control is usually necessary. There are many flea medications available on the market, however, they are not all equally efficacious or safe. Follow the recommendation of your veterinarian by applying a reputable brand of medication as directed, which is commonly once every 30 days. Reputable brands include Revolution®, Bravecto®, Nexgard®, Simparica Trio®, Seresto®, Sentinel®, Trifexis®, and Comfortis®. There are many other brands, however, we recommend consulting your veterinarian before using a new flea product.
Home Care of Hot Spots
Tips for treating a dog’s hot spots include:
- Giving all prescription medication as recommended by your veterinarian.
- Cleaning the affected areas with antibacterial and astringent products daily until healing is complete.
- Making sure that your dog has sufficient water while receiving corticosteroids. House soiling incidents may occur during corticosteroid therapy if the dog is not allowed outdoors on a regular basis.
- Protecting your dog from itching or chewing the areas by using an e-collar, shirt, or bandage.
Preventing Dog Hot Spots
If your dog has a flea allergy and is prone to develop hot spots, you should be aggressive with your flea control program. In addition to treating the environment, you should also apply an appropriate insecticide or repellent to your dog to prevent flea bites. Depending on your area of the country, flea prevention medications are recommended year-round.
Regular bathing, grooming, and clipping of the hair coat can be beneficial in long-haired dogs during the summer months to prevent reoccurrence. It is important to pay particular attention and keep ears clean and dry after swimming or grooming.
Prognosis for Dogs with Hot Spots
The prognosis for dogs with hot spots is very good with appropriate treatment.